
Shared Multi-Omic Data for Advancing Neuroendocrine Neoplasm Research
NETRF-funded researchers have recently reported in the journal GigaScience the first multi-omic dataset of patient-derived

The Neuroendocrine Tumor Research Foundation directs your individual donations to breakthrough scientific research. Since 2005, we have funded $36 million in research projects. The Neuroendocrine Research Foundation is a 501(c)(3) organization, so all donations are fully tax-deductible to the extent allowed by law. We are grateful to you for your generosity.

The Neuroendocrine Tumor Research Foundation directs your individual donations to breakthrough scientific research. Since 2005, we have funded $36 million in research projects. The Neuroendocrine Research Foundation is a 501(c)(3) organization, so all donations are fully tax-deductible to the extent allowed by law. We are grateful to you for your generosity.
 Learn More
Learn More

 Click here to visit the NET Knowledge Center
Click here to visit the NET Knowledge Center

$37.6M
Million in NET research funding
82¢
of every dollar spent in 2022 supported research and education.
50
Ongoing studies in 11 countries

NETRF-funded researchers have recently reported in the journal GigaScience the first multi-omic dataset of patient-derived
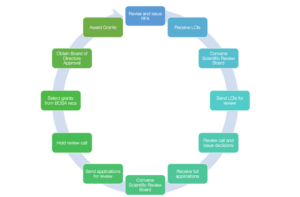
At NETRF, our mission is to fund research that holds promise for advancing the understanding

Recent advancements have broadened the spectrum of treatments for advanced NETs, encompassing a range of
You can support a brighter future. Make a gift. Host an event. Or volunteer to help us advance our understanding of neuroendocrine tumors.
Learn about neuroendocrine tumor tests, treatments, and research. Find out about educational and inspirational events in the NET community.
NETRF hosts free patient and caregiver neuroendocrine tumor conferences to educate and empower individuals to be part of their care planning and live their best life.